Electrocardiogram
February 11, 2015
ELECTROCARDIOGRAM (ECG)
What is an electrocardiogram?
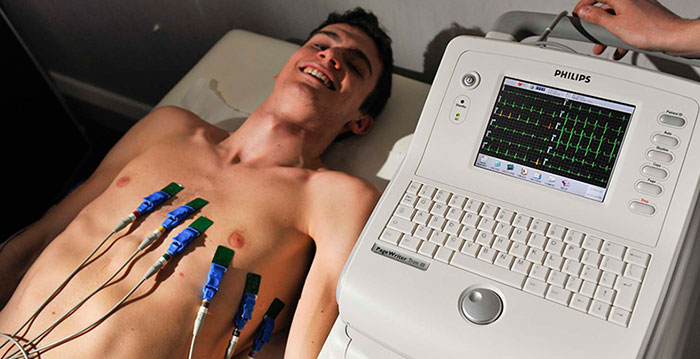
An electrocardiogram (ECG or EKG) is one of the simplest and fastest procedures used to evaluate the heart. Electrodes (small, plastic patches) are placed at certain locations on the chest, arms, and legs. When the electrodes are connected to an ECG machine by lead wires, the electrical activity of the heart is measured, interpreted, and printed out for the doctor's information and further interpretation. Other related procedures that may be used to assess the heart include exercise electrocardiogram (ECG), Holter monitor, signal-averaged ECG, cardiac catheterization, chest X-ray, computed tomography (CT scan) of the chest, echocardiography, electrophysiological studies, magnetic resonance imaging (MRI) of the heart, myocardial perfusion scans, radionuclide angiography, and cardiac CT scan. Please see these procedures for additional information.
The heart's electrical conduction system
The heart is, in the simplest terms, a pump made up of muscle tissue. The heart's pumping action is regulated by an electrical conduction system that coordinates the contraction of the various chambers of the heart. An electrical stimulus is generated by the sinus node (also called the sinoatrial node, or SA node), which is a small mass of specialized tissue located in the right atrium (right upper chamber) of the heart. The sinus node generates an electrical stimulus regularly at 60 to 100 times per minute under normal conditions. This electrical stimulus travels down through the conduction pathways (similar to the way electricity flows through power lines from the power plant to your house) and causes the heart's lower chambers to contract and pump out blood. The right and left atria (the two upper chambers of the heart) are stimulated first and contract a short period of time before the right and left ventricles (the two lower chambers of the heart).
The electrical impulse travels from the sinus node to the atrioventricular node (also called AV node), where impulses are slowed down for a very short period, then continue down the conduction pathway via the bundle of His into the ventricles. The bundle of His divides into right and left pathways to provide electrical stimulation to the right and left ventricles. This electrical activity of the heart is measured by an electrocardiogram. By placing electrodes at specific locations on the body (chest, arms, and legs), a graphic representation, or tracing, of the electrical activity can be obtained. Changes in an ECG from the normal tracing may indicate one or more of several heart-related conditions.
Understanding ECG tracings
Almost everyone knows what a basic ECG tracing looks like. But what does it mean? The first short upward notch of the ECG tracing is called the "P wave." The P wave indicates that the atria (the two upper chambers of the heart) are contracting to pump out blood. The next part of the tracing is a short downward section connected to a tall upward section. This next part is called the "QRS complex." This part indicates that the ventricles (the two lower chambers of the heart) are contracting to pump out blood. The PR interval corresponds to the time measured from the beginning of the P wave to the beginning of the R (or Q) wave. The PR interval indicates the amount of time the electrical impulses take to reach the ventricles from the sinus node. The next short upward segment is called the "ST segment." The ST segment indicates the amount of time from the end of the contraction of the ventricles to the beginning of the rest period before the ventricles begin to contract for the next beat. The next upward curve is called the "T wave." The T wave indicates the resting period of the ventricles. When the doctor views an ECG, he or she studies the size and length of each part of the ECG. Variations in size and length of the different parts of the tracing may be significant. The tracing for each lead of a 12-lead ECG will look different, but will have the same basic components as described above. Each lead of the 12-lead ECG is "looking" at a specific part of the heart, so variations in a lead may indicate a problem with the part of the heart associated with a particular lead.
The video below shows how to read an ECG
Reasons for the procedure
Some reasons for your doctor to request an ECG include, but are not limited to, the following:
- To determine the cause of chest pain
- To evaluate other signs and symptoms which may be heart-related, such as fatigue, shortness of breath, dizziness, or fainting
- o determine the status of the heart prior to procedures such as surgery and/or after treatment for conditions such as a heart attack (myocardial infarction, or MI), endocarditis (inflammation or infection of one or more of the heart valves), or after procedures such as heart surgery or cardiac catheterization
- To assess the function of an implanted pacemaker
- To determine the effectiveness of certain heart medications
- To obtain a baseline tracing of the heart's function during a physical examination that may be used as a comparison with future ECGs, to determine if any changes have occurred
There may be other reasons for your doctor to recommend an ECG.
Risks of the procedure
An ECG is a quick, noninvasive method of assessing the heart’s function. Risks associated with ECG are minimal and rare. Prolonged application of the adhesive electrode patches may cause tissue breakdown or skin irritation at the application site. There may be other risks depending on your specific medical condition. Be sure to discuss any concerns with your doctor prior to the procedure. Certain factors or conditions may interfere with or affect the results of the test. These include, but are not limited to, the following:
- Obesity, pregnancy, or ascites (accumulation of fluid in the abdomen
- Anatomical considerations, such as the size of the chest and the location of the heart within the chest
- Movement during the procedure
- Exercise or smoking prior to the procedure
- Certain medications
- Electrolyte abnormalities, such as too much or too little potassium, magnesium, and/or calcium in the blood
Before the procedure:
- Your doctor or the technician will explain the procedure to you and offer you the opportunity to ask any questions that you might have about the procedure.
- Generally, fasting is not required before the test.
- Notify your doctor of all medications (prescribed and over-the-counter) and herbal supplements that you are taking.
- Notify your doctor if you have a pacemaker.
- Based on your medical condition, your doctor may request other specific preparation.
During the procedure
An ECG may be performed on an outpatient basis or as part of your stay in a hospital. Procedures may vary depending on your condition and your doctor’s practices. Generally, an ECG follows this process:
- You will be asked to remove any jewelry or other objects that may interfere with the procedure.
- You will be asked to remove clothing from the waist up. The technician will ensure your privacy by covering you with a sheet or gown and exposing only the necessary skin.
- You will lie flat on a table or bed for the procedure. It will be important for you to lie still and not talk during the procedure, so as not to interfere with the tracing.
- If your chest, arms, or legs are very hairy, the technician may shave or clip small patches of hair, as needed, so that the electrodes will stick closely to the skin.
- Electrodes will be attached to your chest, arms, and legs.
- The lead wires will be attached to the skin electrodes.
- Once the leads are attached, the technician may key in identifying information about you into the machine's computer.
- The ECG will be started. It will take only a short time for the tracing to be completed.
- Once the tracing is completed, the technician will disconnect the leads and remove the skin electrodes.
After the procedure
You should be able to resume your normal diet and activities, unless your doctor instructs you differently. Generally, there is no special care following an ECG. Notify your doctor if you develop any signs or symptoms you had prior to the test (for example, chest pain, shortness of breath, dizziness, or fainting). Your doctor may give you additional or alternate instructions after the procedure, depending on your particular situation.
Source: www.hopkinsmedicine.org
High Blood Pressure /Hypertension
February 11, 2015
HIGH BLOOD PRESSURE / HYPERTENSION
What is blood pressure?
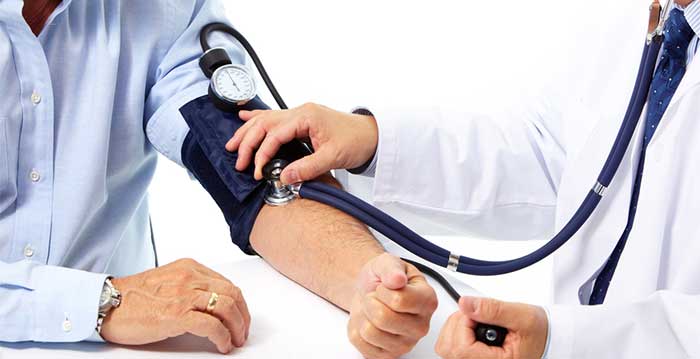
Blood pressure is the force of the blood pushing against the artery walls. The force is generated with each heartbeat as blood is pumped from the heart into the blood vessels. The size and elasticity of the artery walls also affect blood pressure. Each time the heart beats (contracts and relaxes), pressure is created inside the arteries. The pressure is greatest when blood is pumped out of the heart into the arteries or systole. When the heart relaxes between beats (blood is not moving out of the heart), the pressure falls in the arteries or diastole. Two numbers are recorded when measuring blood pressure. The top number, or systolic pressure, refers to the pressure inside the artery when the heart contracts and pumps blood through the body. The bottom number, or diastolic pressure, refers to the pressure inside the artery when the heart is at rest and is filling with blood. Both the systolic and diastolic pressures are recorded as "mm Hg" (millimeters of mercury). This recording represents how high the mercury column in the blood pressure cuff is raised by the pressure of the blood.
Blood pressure is measured with a blood pressure cuff and stethoscope by a nurse or other healthcare provider. A person cannot take his or her own blood pressure unless an electronic blood pressure monitoring device is used High blood pressure, or hypertension, directly increases the risk of coronary heart disease (heart attack) and stroke (brain attack). With high blood pressure, the arteries may have an increased resistance against the flow of blood, causing the heart to pump harder to circulate the blood. Usually, high blood pressure has no signs or symptoms. However, you can know if your blood pressure is high by having it checked regularly by your health care provider. The National Heart, Lung, and Blood Institute (NHLBI) of the National Institutes of Health (NIH) has determined two levels of high blood pressure for adults:
Stage 1
- 140 mm Hg to 159 mm Hg systolic pressure—higher number and
- 90 mm Hg to 99 mm Hg diastolic pressure—lower number
Stage 2
- 160 mm Hg or higher systolic pressure and
- 100 mm Hg or higher diastolic pressure The NHLBI defines prehypertension as:
- 120 mm Hg to 139 mm Hg systolic pressure and
- 80 mm Hg to 89 mm Hg diastolic pressure The NHLBI guidelines define normal blood pressure as follows:
- Less than 120 mm Hg systolic pressure and
- Less than 80 mm Hg diastolic pressure
What are the risk factors for high blood pressure?
Nearly one-third of all Americans have high blood pressure, but it is particularly prevalent in:
- People who have diabetes, gout, or kidney disease
- African Americans (particularly those who live in the southeastern United States
- People in their early to middle adult years; men in this age group have higher blood pressure more often than women in this age group
- People in their middle to later adult years; women in this age group have higher blood pressure more often than men in this age group (more women have high blood pressure after menopause than men of the same age
- Middle-aged and elderly people; more than half of all Americans age 60 and older have high blood pressure
- People with a family history of high blood pressure
- Obese people
- Heavy drinkers of alcohol
- Women who are taking oral contraceptives
How does blood pressure increase?
The following conditions are known to contribute to high blood pressure:
- Being overweight
- Excessive sodium intake (How much salt should you eat?)
- A lack of exercise and physical activity
How is high blood pressure controlled?
High blood pressure can be controlled by:
- Taking prescribed medications exactly as ordered by your health care provider
- Choosing foods that are low in sodium (Can too little salt be harmful?
- Choosing foods high in fiber
- Maintaining a healthy weight, or losing weight if overweight
- Limiting serving sizes
- Increasing physical activity
- Reducing or omitting alcoholic beverages
However, other people must take daily medication to control hypertension. People with hypertension should routinely have their blood pressure checked and be under the care of a physician.
Source: Hopkinsmedicine.org
High Blood Cholesterol
February 12, 2015
HIGH BLOOD CHOLESTEROL
Everyone older than age 20 should get their cholesterol levels measured at least once every five years. High cholesterol does not cause symptoms; so many people are unaware that their cholesterol levels are too high. Lowering cholesterol levels that are too high lessens the risk for developing heart disease and reduces the chance of a heart attack or dying of heart disease, even if you already have it. To assess your cholesterol level, your doctor will usually ask for a simple blood test called a lipoprotein profile. The lipoprotein profile evaluates the following:
- LDL (low density lipoprotein cholesterol, also called "bad" cholesterol)
- HDL (high density lipoprotein cholesterol, also called "good" cholesterol)
- Triglycerides
- Total cholesterol level
Watch the video to learn more about cholesterol in the body
In addition to the blood test, your doctor will perform a full physical exam, discussing your medical history, checking your heart rate, listening to your heartbeat, and taking your blood pressure. If your cholesterol is found to be high, especially if you have other risk factors for heart disease, your doctor will recommend various treatment options ranging from dietary and lifestyle changes to medication to lower your cholesterol. Further tests may be recommended if your doctor feels you are at risk for heart disease.
Source: WebMD
Blood glucose monitoring
February 19, 2015
BLOOD GLUCOSE MONITORING
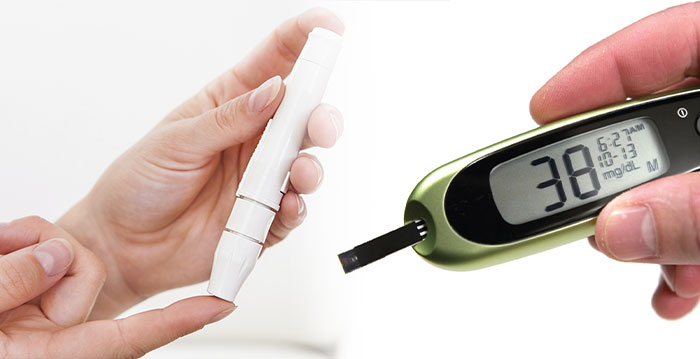
Blood glucose monitoring is a way of testing the concentration of glucose in the blood (glycemia). Particularly important in the care of diabetes mellitus, a blood glucose test is performed by piercing the skin (typically, on the finger) to draw blood, then applying the blood to a chemically active disposable 'test-strip'. Different manufacturers use different technology, but most systems measure an electrical characteristic, and use this to determine the glucose level in the blood. The test is usually referred to as capillary blood glucose. Healthcare professionals advise patients with diabetes on the appropriate monitoring regime for their condition. Most people with Type 2 diabetes test at least once per day. Diabetics who use insulin (all Type 1 diabetes and many Type 2s) usually test their blood sugar more often (3 to 10 times per day), both to assess the effectiveness of their prior insulin dose and to help determine their next insulin dose. Improved technology for measuring blood glucose is rapidly changing the standards of care for all diabetic people.
Purpose
Blood glucose monitoring reveals individual patterns of blood glucose changes, and helps in the planning of meals, activities, and at what time of day to take medications.Also, testing allows for quick response to high blood sugar (hyperglycemia) or low blood sugar (hypoglycemia). This might include diet adjustments, exercise, and insulin (as instructed by the health care provider).
Blood glucose meters
A blood glucose meter is an electronic device for measuring the blood glucose level. A relatively small drop of blood is placed on a disposable test strip which interfaces with a digital meter. Within several seconds, the level of blood glucose will be shown on the digital display. Needing only a small drop of blood for the meter means that the time and effort required for testing is reduced and the compliance of diabetic people to their testing regimens is improved. Although the cost of using blood glucose meters seems high, it is believed to be a cost benefit relative to the avoided medical costs of the complications of diabetes. Recent advances include:
- 'alternate site testing', the use of blood drops from places other than the finger, usually the palm or forearm. This alternate site testing uses the same test strips and meter, is practically pain free, and gives the real estate on the finger tips a needed break if they become sore. The disadvantage of this technique is that there is usually less blood flow to alternate sites, which prevents the reading from being accurate when the blood sugar level is changing.
- 'no coding' systems. Older systems required 'coding' of the strips to the meter. This carried a risk of 'miscoding', which can lead to inaccurate results. Two approaches have resulted in systems that no longer require coding. Some systems are 'autocoded', where technology is used to code each strip to the meter. And some are manufactured to a 'single code', thereby avoiding the risk of miscoding.
- 'multi-test' systems. Some systems use a cartridge or a disc containing multiple test strips. This has the advantage that the user doesn't have to load individual strips each time, which is convenient and can enable quicker testing.
- 'downloadable' meters. Most newer systems come with software that allows the user to download meter results to a computer. This information can then be used, together with health care professional guidance, to enhance and improve diabetes management. The meters usually require a connection cable, unless they are designed to work wirelessly with an insulin pump, or are designed to plug directly into the computer.
Continuous glucose monitoring
A continuous glucose monitor (CGM) determines glucose levels on a continuous basis (every few minutes). A typical system consists of:
- a disposable glucose sensor placed just under the skin, which is worn for a few days until replacement
- a link from the sensor to a non-implanted transmitter which communicates to a radio receiver
- an electronic receiver worn like a pager (or insulin pump) that displays glucose levels with nearly continuous updates, as well as monitors rising and falling trends.
Continuous glucose monitors measure the glucose level of interstitial fluid. Shortcomings of CGM systems due to this fact are:
- continuous systems must be calibrated with a traditional blood glucose measurement (using current technology) and therefore require both the CGM system and occasional "fingerstick"
- glucose levels in interstitial fluid lag behind blood glucose values
Patients therefore require traditional fingerstick measurements for calibration (typically twice per day) and are often advised to use fingerstick measurements to confirm hypo- or hyperglycemia before taking corrective action. The lag time discussed above has been reported to be about 5 minutes. Anecdotally, some users of the various systems report lag times of up to 10–15 minutes. This lag time is insignificant when blood sugar levels are relatively consistent. However, blood sugar levels, when changing rapidly, may read in the normal range on a CGM system while in reality the patient is already experiencing symptoms of an out-of-range blood glucose value and may require treatment. Patients using CGM are therefore advised to consider both the absolute value of the blood glucose level given by the system as well as any trend in the blood glucose levels. For example, a patient using CGM with a blood glucose of 100 mg/dl on their CGM system might take no action if their blood glucose has been consistent for several readings, while a patient with the same blood glucose level but whose blood glucose has been dropping steeply in a short period of time might be advised to perform a fingerstick test to check for hypoglycemia. Continuous monitoring allows examination of how the blood glucose level reacts to insulin, exercise, food, and other factors. The additional data can be useful for setting correct insulin dosing ratios for food intake and correction of hyperglycemia. Monitoring during periods when blood glucose levels are not typically checked (e.g. overnight) can help to identify problems in insulin dosing (such as basal levels for insulin pump users or long-acting insulin levels for patients taking injections). Monitors may also be equipped with alarms to alert patients of hyperglycemia or hypoglycemia so that a patient can take corrective action(s) (after fingerstick testing, if necessary) even in cases where they do not feel symptoms of either condition. While the technology has its limitations, studies have demonstrated that patients with continuous sensors experience less hyperglycemia and also reduce their glycosylated hemoglobin levels. Currently, continuous blood glucose monitoring is not automatically covered by health insurance in the United States in the same way that most other diabetic supplies are covered (e.g. standard glucose testing supplies, insulin, and even insulin pumps). However, an increasing number of insurance companies do cover continuous glucose monitoring supplies (both the receiver and disposable sensors) on a case-by-case basis if the patient and doctor show a specific need. The lack of insurance coverage is exacerbated by the fact that disposable sensors must be frequently replaced. Some sensors have been U.S. Food and Drug Administration (FDA) approved for 7- and 3-day use, though some patients wear sensors for longer than the recommended period) and the receiving meters likewise have finite lifetimes (less than 2 years and as little as 6 months). This is one factor in the slow uptake in the use of sensors that have been marketed in the United States.
Video how to test your blood glucose (sugar) levels
Glucose sensing bio-implants
Investigations on the use of test strips have shown that the required self-injury acts as a psychological barrier restraining the patients from sufficient glucose control. As a result, secondary diseases are caused by excessive glucose levels. A significant improvement of diabetes therapy might be achieved with an implantable sensor that would continuously monitor blood sugar levels within the body and transmit the measured data outside. The burden of regular blood testing would be taken from the patient, who would instead follow the course of their glucose levels on an intelligent device like a laptop or a smart phone. Glucose concentrations do not necessarily have to be measured in blood vessels, but may also be determined in the interstitial fluid, where the same levels prevail – with a time lag of a few minutes – due to its connection with the capillary system. However, the enzymatic glucose detection scheme used in single-use test strips is not directly suitable for implants. One main problem is caused by the varying supply of oxygen, by which glucose is converted to glucono lactone and H2O2 by glucose oxidase. Since the implantation of a sensor into the body is accompanied by growth of encapsulation tissue,[10] the diffusion of oxygen to the reaction zone is continuously diminished. This decreasing oxygen availability causes the sensor reading to drift, requiring frequent re-calibration using finger-sticks and test strips. One approach to achieving long-term glucose sensing is to measure and compensate for the changing local oxygen concentration. Other approaches replace the troublesome glucose oxidase reaction with a reversible sensing reaction, known as an affinity assay. This scheme was originally put forward by Schultz and Sims in 1978. A number of different affinity assays have been investigated, with fluorescent assays proving most common. MEMS technology has recently allowed for smaller and more convenient alternatives to fluorescent detection, via measurement of viscosity. Investigation of affinity-based sensors has shown that encapsulation by body tissue does not cause a drift of the sensor signal, but only a time lag of the signal compared to the direct measurement in blood.
Non-invasive technologies
Some new technologies to monitor blood glucose levels will not require access to blood to read the glucose level. Non-invasive technologies include near IR detection, ultrasound and dielectric spectroscopy. These will free the person with diabetes from finger sticks to supply the drop of blood for blood glucose analysis. Most of the non-invasive methods under development are continuous glucose monitoring methods and offer the advantage of providing additional information to the subject between the conventional finger stick, blood glucose measurements and over time periods where no finger stick measurements are available (i.e. while the subject is sleeping).
Effectiveness
For patients with diabetes mellitus type 2, the importance of monitoring and the optimal frequency of monitoring are not clear. A 2011 study found no evidence that blood glucose monitoring leads to better patient outcomes in actual practice. One randomized controlled trial found that self-monitoring of blood glucose did not improve glycosylated hemoglobin (HbA1c) among "reasonably well controlled non-insulin treated patients with type 2 diabetes".[23] However a recent meta-analysis of 47 randomized controlled trials encompassing 7677 patients showed that self-care management intervention improves glycemic control in diabetics, with an estimated 0.36% (95% CI, 0.21-0.51) reduction in their glycosylated hemoglobin values. Furthermore, a recent study showed that patients described as being “Uncontrolled Diabetics” (defined in this study by HbA1C levels >8%) showed a statistically significant decrease in the HbA1C levels after a 90-day period of seven-point self-monitoring of blood glucose (SMBG) with a relative risk reduction (RRR) of 0.18%. Regardless of lab values or other numerical parameters, the purpose of the clinician is to improve quality of life and patient outcomes in diabetic patients. A recent study included 12 randomized controlled trials and evaluated outcomes in 3259 patients. The authors concluded through a qualitative analysis that SMBG on quality of life showed no effect on patient satisfaction or the patients’ health-related quality of life. Furthermore, the same study identified that patients with type 2 diabetes mellitus diagnosed greater than one year prior to initiation of SMBG, who were not on insulin, experienced a statistically significant reduction in their HbA1C of 0.3% (95% CI, -0.4 - -0.1) at six months follow up, but a statistically insignificant reduction of 0.1% (95% CI, -0.3 – 0.04) at twelve months follow up. Conversely, newly diagnosed patients experienced a statistically significant reduction of 0.5% (95% CI, -0.9 – -0.1) at 12 months follow up. A recent study found that a treatment strategy of intensively lowering blood sugar levels (below 6%) in patients with additional cardiovascular disease risk factors poses more harm than benefit. For type 2 diabetics who are not on insulin, exercise and diet are the best tools. Blood glucose monitoring is, in that case, simply a tool to evaluate the success of diet and exercise. Insulin-dependent type 2 diabetics need to monitor their blood sugar as frequently as type 1 diabetics.
Magnetic Resonance Imaging (MRI Scan)
February 22, 2015
MAGNETIC RESONANCE IMAGING (MRI SCAN)
MRI scan facts
- MRI scanning uses magnetism, radio waves, and a computer to produce images of body structures.
- MRI scanning is painless and does not involve x-ray radiation.
- Patients with heart pacemakers, metal implants, or metal chips or clips in or around the eyes cannot be scanned with MRI because of the effect of the magnet.
- Claustrophobic sensation can occur with MRI scanning.
What is an MRI scan?
An MRI (or magnetic resonance imaging) scan is a radiology technique that uses magnetism, radio waves, and a computer to produce images of body structures. The MRI scanner is a tube surrounded by a giant circular magnet. The patient is placed on a moveable bed that is inserted into the magnet. The magnet creates a strong magnetic field that aligns the protons of hydrogen atoms, which are then exposed to a beam of radio waves. This spins the various protons of the body, and they produce a faint signal that is detected by the receiver portion of the MRI scanner. The receiver information is processed by a computer, and an image is produced. The image and resolution produced by MRI is quite detailed and can detect tiny changes of structures within the body. For some procedures, contrast agents, such as gadolinium, are used to increase the accuracy of the images.
When are MRI scans used?
An MRI scan can be used as an extremely accurate method of disease detection throughout the body and is most often used after the other testing fails to provide sufficient information to confirm a patient's diagnosis. In the head, trauma to the brain can be seen as bleeding or swelling. Other abnormalities often found include brain aneurysms, stroke, tumors of the brain, as well as tumors or inflammation of the spine. Neurosurgeons use an MRI scan not only in defining brain anatomy but in evaluating the integrity of the spinal cord after trauma. It is also used when considering problems associated with the vertebrae or intervertebral discs of the spine. An MRI scan can evaluate the structure of the heart and aorta, where it can detect aneurysms or tears. MRI scans are not the first line of imaging test for these issues or in cases of trauma. It provides valuable information on glands and organs within the abdomen, and accurate information about the structure of the joints, soft tissues, and bones of the body. Often, surgery can be deferred or more accurately directed after knowing the results of an MRI scan.
What are the risks of an MRI scan?
An MRI scan is a painless radiology technique that has the advantage of avoiding x-ray radiation exposure. There are no known side effects of an MRI scan. The benefits of an MRI scan relate to its precise accuracy in detecting structural abnormalities of the body. Patients who have any metallic materials within the body must notify their physician prior to the examination or inform the MRI staff. Metallic chips, materials, surgical clips, or foreign material (artificial joints, metallic bone plates, or prosthetic devices, etc.) can significantly distort the images obtained by the MRI scanner. Patients who have heart pacemakers, metal implants, or metal chips or clips in or around the eyeballs cannot be scanned with an MRI because of the risk that the magnet may move the metal in these areas. Similarly, patients with artificial heart valves, metallic ear implants, bullet fragments, and chemotherapy or insulin pumps should not have MRI scanning.
During the MRI scan, patient lies in a closed area inside the magnetic tube. Some patients can experience a claustrophobic sensation during the procedure. Therefore, patients with any history of claustrophobia should relate this to the practitioner who is requesting the test, as well as the radiology staff. A mild sedative can be given prior to the MRI scan to help alleviate this feeling. It is customary that the MRI staff will be nearby during MRI scan. Furthermore, there is usually a means of communication with the staff (such as a buzzer held by the patient) which can be used for contact if the patient cannot tolerate the scan.
How does a patient prepare for an MRI scan and how is it performed?
All metallic objects on the body are removed prior to obtaining an MRI scan. Occasionally, patients will be given a sedative medication to decrease anxiety and relax the patient during the MRI scan. MRI scanning requires that the patient lie still for best accuracy. Patients lie within a closed environment inside the magnetic machine. Relaxation is important during the procedure and patients are asked to breathe normally. Interaction with the MRI technologist is maintained throughout the test. There are loud, repetitive clicking noises which occur during the test as the scanning proceeds. Occasionally, patients require injections of liquid intravenously to enhance the images which are obtained.The MRI scanning time depends on the exact area of the body studied, but ranges from half an hour to an hour and a half.
Video How Does an MRI Machine Work
How does a patient obtain the results of the MRI scan?
After the MRI scanning is completed, the computergenerates visual images of the area of the body that was scanned.These images can be transferred to film (hard copy). A radiologist is a physician who is specially trainedto interpret images of the body. The interpretation is transmitted in the form of a report to the practitioner whorequested the MRI scan. The practitioner can then discuss theresults with the patient and/or family.
Future
Scientists are developing newer MRI scanners that are smaller, portable devices. These new scanners apparently can be most useful in detecting infections and tumors of the soft tissues of the hands, feet, elbows, and knees. The application of these scanners to medical practice is now being tested.
Chronic obstructive pulmonary disease (COPD)
February 22, 2015
CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD)
Chronic obstructive pulmonary disease (COPD) describes a number of long-term lung conditions that cause breathing difficulties. It’s estimated that about one million people in the UK have COPD and that there are many more who haven’t been diagnosed. It’s the fifth most common cause of death in England and Wales with about 28,000 people dying as a result of it every year. You’re more likely to develop the condition as you get older. COPD is usually caused by smoking and tends to get progressively worse over time.
The term COPD describes a number of conditions but the most common are chronic bronchitis and emphysema.
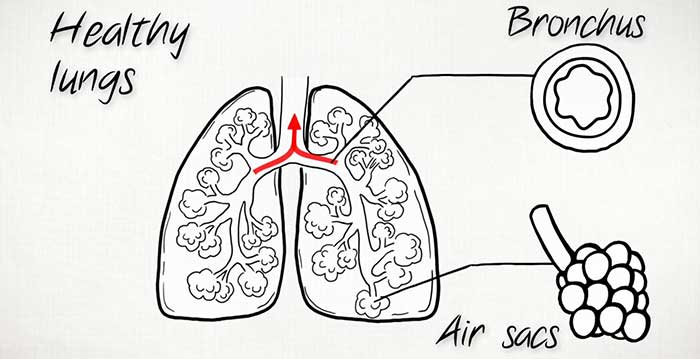
- Chronic bronchitis is caused by inflammation of your bronchi – these are the main airways that lead from your windpipe (trachea) to your lungs. This inflammation can lead to excess mucus that may block your airways.
- Emphysema is the term used to describe damage to the walls of your alveoli. These are tiny air sacs in your lungs where oxygen passes into your blood.
The damage to your lungs means that less oxygen passes into your blood to be transported around your body to your tissues, including your brain. This contributes to symptoms such as having difficulty breathing and tiredness.
Symptoms of COPD
At first, you may not have any symptoms of COPD or they may be very mild. The condition may start with either a persistent, phlegmy cough or breathlessness. Many people don’t see their GP at this early stage, but the earlier you get advice and treatment the better. As COPD progresses symptoms can vary but may also include:
- persistent cough
- breathlessness with physical exertion
- regularly coughing up phlegm
- wheezing
- weight loss
- extreme tiredness
- waking up at night as a result of breathlessness
- swollen ankles
You may find your symptoms are worse in the winter months. These symptoms aren’t always caused by COPD but if you have them, see your GP. It isn’t usual to get chest pains or cough up blood if you have COPD. If this happens, you may either have something other than COPD or another condition as well as COPD.
Diagnosis
Your GP will ask about your symptoms and will ask to examine you. He or she is likely to ask you if you smoke and if there are any other reasons why you may be at risk of COPD. Your GP may ask to listen to your chest with a stethoscope to see if you have any wheezing or crackling sounds when you breathe. There is no single test that can confirm COPD. If your GP thinks you may have it, he or she may advise you to have a lung spirometry test. This tests how well your lungs are working. Your GP will ask you to blow into a device that measures how much and how quickly you can force out air from your lungs. Different lung problems produce different results so this helps to separate COPD from other chest conditions. For more information see our frequently asked questions. Other tests you may be offered are listed below.
- A chest X-ray to see if your lungs show signs of COPD, and to exclude other lung diseases.
- A blood test to look for anaemia or signs of infection.
If you’re diagnosed with COPD, your doctor may advise you to have further tests. These will help to determine the best treatment for you.
- A CT (computed tomography) scan to produce three-dimensional images of your lungs.
- An ECG (electrocardiogram) to measure the electrical impulses from your heart to see how well it’s working.
- An echocardiogram to look at the structure and function of your heart.
- Pulse oximetry to monitor the amount of oxygen in your blood to see if you need oxygen therapy.
- An alpha-1 antitrypsin test to see if you have a lack of this protein. You may need this if your COPD developed when you were 40 or younger, or if you don’t smoke.
Treatment of COPD
There are a number of treatment options for COPD, as described below. Which treatments you are offered will depend on your personal circumstances. Your doctor will discuss these with you to help you make a decision that’s right for you. Your decision will be based on your doctor’s expert opinion and your own personal values and preferences. There isn’t a cure for COPD and it isn’t possible to reverse the damage to your lungs. However, there are ways to treat the symptoms and prevent COPD from getting worse. If you smoke, the most important thing you can do is stop. Giving up smoking can relieve your symptoms and slow down the progression of COPD, even if you have had it for a long time. Speak to your GP about ways to give up smoking. Treatment for COPD will vary depending on how severe your condition is. You may be able to manage your condition with self-help measures. However, if it’s more severe or progresses, you may be offered medicines or oxygen therapy.
Self-help
There are other steps you can take to try to prevent COPD from getting worse and to ease your symptoms. Some examples are listed below.
- Make sure you drink enough fluid as this can help to reduce the thickness of mucus that your lungs produce.
- Try to exercise regularly, even if you feel tired. Walking for 20 to 30 minutes at least three times a week is recommended. If you can’t move around, exercise by stretching out your arms and twisting your upper body. See our frequently asked questions for more information.
- Make sure you eat a healthy, balanced diet. It’s important that you eat enough as this will help to prevent your symptoms from getting worse. Your GP may recommend that you take nutritional supplements. See our frequently asked questions for more information.
- Have a flu vaccination each year, and have the vaccination for the Streptococcus pneumoniae bacterium that causes pneumonia.
Pulmonary rehabilitation
This is a scheme that involves exercise, education about COPD, advice on nutrition and psychological support. Pulmonary rehabilitation aims to help reduce your symptoms and make it easier for you to do everyday activities. It’s a good idea to ask your GP about pulmonary rehabilitation and whether there is a programme in your area.
Video COPD
Medicines
There are various medicines that may help to ease your symptoms or control flare-ups. Discuss with your GP which medicine is best for you. You may be advised to take more than one. Some of these medicines are also used to treat asthma.
Bronchodilators
These medicines are commonly used to treat COPD. They widen your airways so air flows through them more easily and can relieve wheezing and breathlessness. They are available as short-acting or long-acting inhalers. There are many different types of bronchodilators – examples include salbutamol, salmeterol and tiotropium.
Steroids
Steroid medicines may help if you have more severe COPD or if a bronchodilator hasn’t helped. Steroids work by reducing inflammation of your airways. They are available as inhalers or tablets. You’re likely to be offered an inhaler if you need to take steroids frequently. Generally you will only be advised to take these tablets for a limited period of time, for example to treat a flare-up. This is because they can cause side-effects if taken regularly. You’re unlikely to be offered a steroid inhaler if your condition is mild. This is because they may increase the risk of pneumonia in some people.
Mucolytics
Mucolytics break down the phlegm and mucus produced by your lungs, making it easier for you to cough it up. Your GP may advise you to take a mucolytic if you develop a persistent, phlegm-producing cough.
Oxygen therapy
If your COPD becomes severe, you may develop a low blood oxygen level. Oxygen therapy can help to relieve this and improve symptoms in some people. You inhale oxygen through a mask or small tubes (nasal cannulae) that sit beneath your nostrils. The oxygen is provided in cylinders for you to use at home or in smaller, portable versions for outside the home. If you need oxygen for long periods of the day (over eight hours), you may be offered an oxygen concentrator. This is a machine that filters out oxygen from the air in the environment and stores it for you to use. You must not smoke if you have oxygen therapy for COPD because there is a serious fire risk. You may not be prescribed oxygen therapy if you haven’t given up smoking. Oxygen therapy can be short-term, long-term (you use it all the time at home) or ambulatory (you use it for exercise or when you’re outdoors). You will probably only be offered oxygen after an appointment with a doctor who specialises in respiratory medicine (identifying and treating conditions of the lungs). You may also need additional oxygen if you travel by air. It’s important to speak to your GP if you have COPD and are considering travelling by plane.
Surgery
If you have severe COPD, your doctor may recommend surgery to remove diseased areas of your lungs. This can help your lungs to function better. However, it’s only carried out in certain circumstances – speak to your doctor for more advice.
Causes of COPD
The biggest single cause of COPD is smoking. If you stop smoking, your risk of developing COPD begins to fall. If you already have COPD, stopping smoking means your symptoms progress more slowly. Other less common causes of COPD include:
- passive smoking
- being exposed to certain chemicals or fumes
- environmental factors, such as air pollution
There are likely to be a number of genetic factors that may increase your risk of COPD but more evidence is needed. It’s known that inheriting a shortage of a protein called alpha-1 antitrypsin, which helps protect your lungs, can increase your risk of COPD. However, fewer than one in 100 people with the condition have this shortage. Smoking also exacerbates the effect of other causes on your risk of developing COPD.
Prevention of COPD
You have the best chance of preventing COPD if you don’t smoke. If your job exposes you to dust or fumes, it’s important to take care at work and use any relevant protective equipment. For example, you may need to wear a face mask to help prevent you from inhaling any harmful substances.
Spirometry Tests
February 23, 2015
SPIROMETRY TESTS
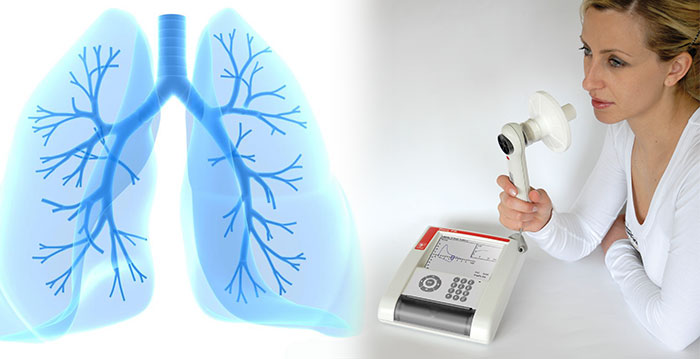
Spirometry is the best test to assess lung function. It often is used to evaluate a person who has a chronic cough and sputum (mucus) production and a history of risk factors for chronic obstructive pulmonary disease (COPD), even if shortness of breath is not present. It is also used to find out whether a specific therapy has improved lung function or whether your lung disease is getting worse. Spirometry testing may be done in your doctor's office or in a hospital. During the test:
- A tube is connected to the spirometer.
- You place your mouth on the tube and take the deepest breath possible.
- You then blow out as hard and as fast as possible.
This should be repeated several times during the visit to ensure accurate results. This test measures the flow and amount of air when you breathe in and out as deeply and forcefully as you can. For people with COPD, the test is divided into:
- Forced expiratory volume in 1 second (FEV1), the amount of air breathed out as forcefully as possible in 1 second. The FEV1 value can help your doctor estimate the severity of COPD.
- Forced vital capacity (FVC), the amount of air that can be forcibly breathed out after taking a deep breath.
Video Spirometry Test
The normal values for each of the measurements depend on your age, height, gender, and race. This is known as the predicted value. People with COPD typically have a reduction in FEV1 and may also have a reduction in FVC. A reduction in the ratio of FEV1 to the FVC points to airway obstruction, including COPD and asthma. These measurements help doctor diagnose COPD and find out the severity of the disease.
What is Body Mass Index (BMI)?
March 6, 2015
WHAT IS BODY MASS INDEX (BMI)?
Healthcare professionals around the world often use Body Mass Index (BMI) when determining whether patients are underweight, healthy weight, overweight or clinically obese. People who are clinically obese have a greater risk of developing diabetes, stroke, some cancer, and cardiovascular diseases. BMI has its drawbacks however. It does not take into account the patient's body fat content versus lean tissue (muscle) content. A 6 feet 2 inch athlete may have a higher BMI than a couch potato of the same height - but the couch potato may be overweight while the athlete is definitely not.
How to calculate BMI - Adults
There are two methods for working out your BMI - metric and imperial systems.
Metric system - Divide the person's weight in kilograms by their height in meters squared.
For example:
- Weight 90 kilograms
- Weight 90 kilograms
- Height 1.9 meters
- 1.9x1.9 = 3.61
- 90 divided by 3.61 = BMI is 24.93
How to determine your body weight status
Below are definitions recommended by the World Health Organization.
BMI less than 18.5 - Underweight
BMI between 18.5 and 25 - Healthy weight
BMI between 25 and 30 - Overweight
BMI between 30 and 40 - Obese
BMI over 40 - Very obese, morbidly obese
Video: How to calculate BMI
BMI definitions vary across countries
Classifying a person's body weight status according to BMI may vary depending on the country that the patient resides. In Japan, for example, a health body weight is defined as a BMI of between 18.5 and 22.9, overweight from 23 to 24.9, and anything over 25 is obese. Up to 1998, US health authorities considered a healthy body weight as up to a BMI of 27. In 1998, the NIH (National Institutes of Health), USA, adopted the World Health Organizations guidelines. Twenty-five million Americans instantly switched from being a healthy weight to overweight from one day to the next when the change came into effect. Before 1998, a person with a BMI of 26.8 would have been classified as a "healthy weight" person in the USA and "obese" in Japan. Nick Trefethen, from Oxford University's Mathematical Institute, explained that the problem with the BMI formula is that humans do not grow equally in all three dimensions. He has come up with what he believes is a better formula than the BMI one for determining whether somebody is carrying too much fat.
BMI Classifications (International)
BMI of less than 18.5kg/m2
A BMI of less than 18.5 indicates that you are underweight, so you may need to put on some weight. You are recommended
to ask your Doctor or a dietician for advice.
BMI of 18.5 - 25kg/m2
A BMI of 18.5 - 25 indicates that you are at a healthy weight for your height. By maintaining a healthy weight, you lower your risk of developing serious health problems.
BMI of 25 - 30kg/m2
A BMI of 25 - 30 indicates that you are slightly overweight. You may be advised to lose some weight for health
reasons. You are recommended to talk to your Doctor or a dietician for advice.
BMI of over 30kg/m2
A BMI of over 30 indicates that you are heavily overweight. Your health may be at risk if you do not lose weight. You are
recommended to talk to your Doctor or a dietician for advice.
Note:
The results given by the BMI calculator should be used only as a guide and should not replace medical advice. Please bear in mind that, as mentioned in our article, when
interpreting the results of the body mass index calculator, other factors such as muscle structure and ethnic origin should be considered.
Always speak to a Doctor or health professional for advice and guidance before making any dramatic changes to your lifestyle.